08 Dec Tooth Extractions & Denture Essentials
Dental health is a crucial component of overall well-being, and sometimes, preserving this health means making the difficult decision to remove a tooth. Whether precipitated by unremitting decay, the consequences of periodontal disease, the strategic requirements of orthodontics, or the complications arising from impacted teeth, the biological rationale for tooth extraction is both complex and vital for one’s continued health. This essay delves into the scientific underpinnings that render tooth extraction necessary, exploring the pathophysiology behind dental impairments and the potential risks of ignoring such issues. As we navigate through the intricate processes and techniques of tooth removal and consider the subsequent journey to obtaining and maintaining dentures, we offer a comprehensive guide to this often inevitable dental journey, equipping individuals with the knowledge needed to approach these experiences with confidence.
Biological Rationale for Tooth Extraction
The Imperative of Tooth Extraction in Dental Medicine
The ideal in dental practice is undoubtedly the preservation of natural dentition; however, tooth extraction remains a pivotal procedure within the spectrum of oral healthcare. The necessity of this intervention may appear counterintuitive given the advancements in dental medicine aimed at conservation. Nevertheless, understanding the underlying rationale for tooth extraction is intrinsic to grasping the complexities of maintaining oral health and systemic well-being.
Tooth extraction can be considered a last resort, necessitated only when alternative treatments cannot restore the structural integrity or alleviate the pathology afflicting the tooth. The etiologies warranting extraction are diverse and multifaceted, each sharing the commonality of an impasse where the potential detriments of retaining the tooth overshadow the benefits.
Endodontic failures provide a clear illustration of such circumstances. Teeth that have undergone root canal treatment may occasionally succumb to recurrent infections or persistent disease. In these instances, the structural compromise of the tooth, combined with the risk of harboring bacteria resistant to endodontic therapy, might necessitate extraction to prevent further infection and systemic spread.
Periodontal disease represents another leading cause prompting tooth extraction. Advanced periodontitis can result in the irreversible loss of supportive alveolar bone and periodontal ligament. When a tooth becomes excessively mobile and functional integrity is compromised, its extraction is not only beneficial but imperative to prevent adjacent teeth from enduring similar fates due to the continued inflammatory insult.
Impaction–commonly seen with third molars, or ‘wisdom teeth’–is a state in which teeth fail to erupt adequately or assume a functional position in the dental arch. Impacted teeth can precipitate a slew of complications, including cyst formation, resorption of adjacent teeth, and the exacerbation of crowding. Prophylactic extraction of impacted teeth is at times advocated to circumvent these potentially deleterious outcomes.
In orthodontics, the strategic removal of certain teeth, primarily premolars, can be pivotal for successful space management and the correction of malocclusions. The extraction of these teeth in a controlled manner enables the reharmonization of dental and facial esthetics through subsequent alignment procedures.
Oncologic concerns substantiate the necessity of extraction in certain diagnoses. Oral cancers, as well as their respective treatment protocols, may render teeth nonviable. The removal of these teeth is integral to the broader therapeutic strategy, which may encompass surgical, chemotherapeutic, or radiation treatments.
Furthermore, pathologic conditions such as dental caries can progress to such an extent that restoration is implausible. When the structure of a tooth is subverted and the invasion of bacteria into the pulp is unchecked, the risk of abscess formation, localized osteitis, and more generalized infection necessitates the prompt removal of the tooth in question.
Thus, while the practice of dental extraction might superficially appear antithetical to the conservationist goals of modern dentistry, it remains grounded in a pragmatic approach to patient care. The judgment to prescribe extraction derives from a meticulous assessment of the tooth’s prognostic outlook and its systemic implications. This clinical decision should not be perceived as a failure but as a discerning measure to uphold the integrity and health of the oral cavity and the patient as a whole.
Processes and Techniques in Tooth Extraction
In the realm of dental surgery, the execution of tooth extractions necessitates a profound adherence to best practices to ensure optimal patient outcomes and procedural efficacy. This discourse aims to elucidate the paramount protocols that underscore current best practices for tooth extraction, a nuanced undertaking that directly interfaces with the systemic health and wellness of dental patients.
Foremost, it is incumbent upon the dental surgeon to conduct a comprehensive preoperative evaluation. This encompasses a meticulous review of the patient’s medical and dental histories, coupled with diagnostic imaging to discern the exact position, condition, and structural integrity of the tooth and surrounding tissues. Digital radiography, including periapical, panoramic, and, when indicated, cone beam computed tomography (CBCT) scans, afford critical insight into potential anatomical impediments such as proximity to vital structures like the inferior alveolar nerve or the maxillary sinus.
In the operative phase, anesthesia constitutes a critical component, with the objective of ensuring a pain-free procedure. Local anesthesia, often augmented with a vasoconstrictor, extends the duration of numbness, while minimizing bleeding. Anxiolytics or sedation may be employed for patients exhibiting dental anxiety, thus fostering a tranquil operational milieu.
The adoption of atraumatic surgical techniques inextricably links to the preservation of bony structures and the mitigation of postoperative discomfort. A dexterous approach involves initial gingival incision followed by the judicious use of elevators to luxate the tooth, thereby minimizing force and thus the risk of fracture to both the tooth and the alveolar bone. Dental forceps, adapted to the tooth’s configuration, facilitate removal once the tooth has sufficiently mobilized. For multi-rooted teeth, sectioning the tooth may be requisite, providing an avenue to remove each root individually and preserve bone.
During the procedure, hemostasis is of paramount importance, attainable via direct pressure, the application of hemostatic agents, or suturing. Mastery in bleeding management not only promotes patient comfort but also deters the development of postoperative complications, such as hematoma formation.
Post extraction, socket preservation strategies spring to the fore, with close attention to the prospect of subsequent prosthetic or implant rehabilitation. Practitioners might exercise the option of employing bone grafting materials or barrier membranes to foster an advantageous osseous landscape for future dental prostheses.
Pain management in the postoperative juncture must not be understated. Explicit instructions on the judicious use of analgesics and non-steroidal anti-inflammatory drugs (NSAIDs) are imparted, with attention to the patient’s medical history and potential drug interactions. Additionally, prudent advice on home care — inclusive of cold compress application, maintenance of oral hygiene, and dietary adjustments — is dispensed to accentuate healing and forestall complications such as alveolar osteitis, or dry socket.
In circumspect, adherence to these best practices in tooth extraction is not merely a provision of care but rather an embodiment of surgical artistry and scientific acumen. It is a process characterized by precision, forethought, and a staunch commitment to the overarching ethos of patient welfare and preservation of oral health.
Photo by dentistozkanguner on Unsplash
Transitioning from Natural Teeth to Dentures
Transitioning to dentures represents a significant adaptation phase for patients who have undergone dental extractions. The process to ensure an effective transition hinges on meticulous planning, starting with the selection of appropriate denture types—be it complete, partial, immediate, or overdentures.
Upon tooth removal, immediate dentures can offer the benefit of preserving aesthetics and function, albeit temporary, until the patient’s tissues heal. However, the fundamental premise is the healing process post-extraction; the residual ridge needs time and care to recover to provide a stable foundation for the denture. The alveolar bone remodeling period typically extends over several months post-extraction, during which interim liners or tissue conditioners play a crucial role in maintaining denture fit and comfort.
Alveolar ridge preservation is another critical facet of this transition. It mitigates the loss of bone volume and density that accompanies tooth removal, employing techniques such as socket grafting with bone substitutes and guided bone regeneration. Such interventions are designed to optimize the ridge morphology, enhancing subsequent prosthetic outcomes.
Adequate soft tissue management is also essential. It involves ensuring a healthy keratinized gingival margin and reducing surgical trauma to preserve vascularity and facilitate subsequent tissue adaptation to dentures. Patients should be guided on maintaining impeccable oral hygiene to prevent prosthodontic stomatitis and other mucosal lesions.
Furthermore, the fabrication process of the definitive dentures is intricate, requiring accurate impressions that capture the nuanced topography of the edentulous ridges and surrounding tissues. Jaw relation records are essential to establish the correct occlusal relationships, facilitating proper masticatory function and minimizing the risk of temporomandibular disorders.
The material selection for dentures also holds paramount importance, considering factors such as biocompatibility, durability, esthetics, and ease of repair. Technological advancements, such as CAD/CAM dentures and the incorporation of resilient liner materials, have elevated the functional and aesthetic benchmarks of denture prosthetics.
Patient education is indispensable throughout this transition. Gradual acclimatization to new sensory experiences, such as the taste, temperature, and occlusal force distribution, is often necessary. Nutritional counseling and adaptation to new chewing patterns can help maintain overall health.
Finally, regular follow-up appointments are essential to assess tissue health, check for pressure sores, adjust occlusion, and evaluate the need for reline procedures. These appointments also provide an opportunity for continuous reinforcement of proper denture maintenance and handling techniques.
In assembling the complexities of transitioning to dentures post-extractions, a multi-disciplinary approach is often advantageous. Collaboration with dental technologists, hygienists, and sometimes even speech therapists enrich the standard of care. This holistic approach to prosthodontic rehabilitation ensures that patients regain not only function and esthetics but also confidence and quality of life after the loss of natural dentition.
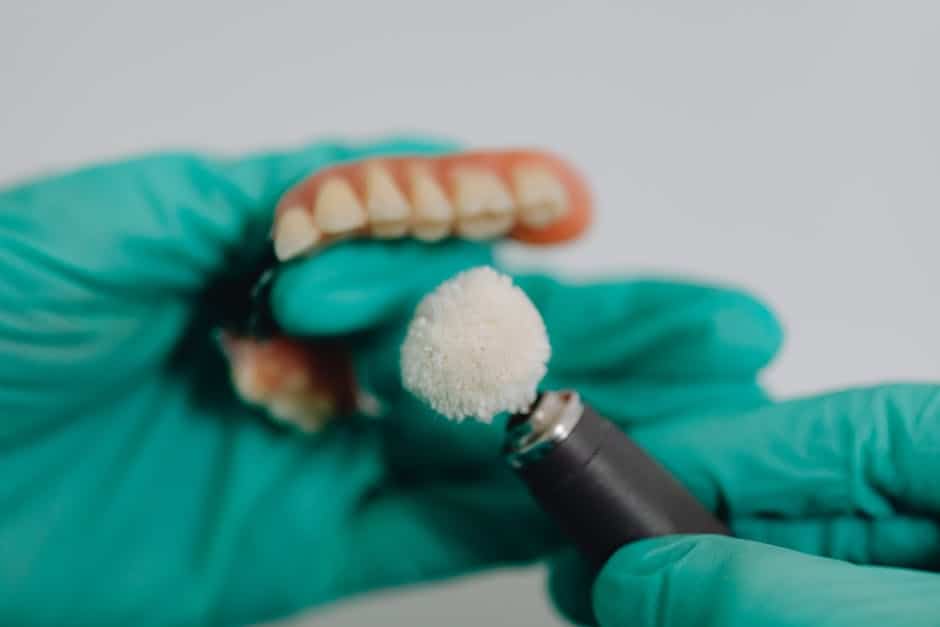
Long-Term Care and Maintenance of Dentures
Maintaining optimal denture health requires a steadfast commitment to oral hygiene and routine care practices. A crucial element in prolonging the life and functionality of dentures is the meticulous and regular cleaning of the prosthesis. This routine not only preserves the aesthetic appearance but also prevents the accumulation of debris and microbial plaque that could lead to irritation and infection of the oral mucosa, a condition often referred to as denture stomatitis.
The choice of cleansing agents must be made judiciously. It is recommended to use a soft-bristle brush specifically designed for dentures, alongside non-abrasive denture cleansers that effectively remove food particles and stains without damaging the denture material. Immersing dentures in a mild alkaline peroxide-based effervescent solution can assist in dislodging adherent deposits and reducing microbial load.
Furthermore, denture wearers must take heed to engage in regular diligent care of the remaining oral tissues. This includes brushing the gums, tongue, and palate daily with a soft-bristled brush prior to inserting the dentures. Such a practice stimulates circulation in the tissues and helps reduce the risk of oral infections.
An often neglected aspect of denture maintenance is the need for periodic adjustments. As the oral anatomy inevitably changes due to bone resorption and tissue remodeling, dentures may lose their fit, resulting in discomfort and functional impairment. Hence, it is imperative for patients to schedule regular visits with their dental professionals for adjustments, relines, or rebasing of their dentures. The aforementioned interventions aim to adapt the denture base to the current contour of the alveolar ridges, thereby ensuring continued comfort, function, and stability.
Moreover, while nocturnal denture wear is sometimes advocated for specific therapeutic reasons, the prevailing guidance is for patients to discontinue wearing dentures during sleep. This practice diminishes the risk of microbial proliferation and allows the oral mucosa a necessary period for reprieve and aeration, fundamentally reducing the risk of both soft tissue irritation and bone resorption.
Lastly, even with rigorous maintenance of dentures and adherence to optimal hygiene protocols, the longevity of a denture is finite. Material fatigue, wear, and the dynamic nature of the oral environment necessitate eventual replacement of the prosthesis. Acknowledgement of this eventuality underscores the importance of ongoing communication between dental practitioners and their patients, fostering an environment where prosthodontic needs are anticipated and met with prompt and effective intervention.
In summation, denture health is a multifactorial endeavor, predicated on thorough cleaning, attentive tissue care, timely professional adjustments, judicious wear practices, and the recognition of the natural lifecycle of the prosthetic device. Mastery of these guidelines equips denture wearers with the essential tools for preserving oral health and ensuring that their dental prostheses serve them well for the duration of their use.
Maintaining a healthy smile is a lifelong commitment that doesn’t end with tooth extraction—it merely transitions into a different phase of care. For those embarking on the denture journey, understanding the importance of detail-oriented maintenance is paramount to ensure oral health and the longevity of one’s dental prosthesis. From the meticulous cleaning routines to the routine adjustments necessitated by natural anatomical changes, this guide has offered an enlightening perspective on the road that lies ahead for denture wearers. However challenging the initial adjustment may be, the advances in modern dentistry promise a future where dentures not only restore function but also provide comfort and confidence, enabling individuals to continue to smile without hesitation.


Sorry, the comment form is closed at this time.